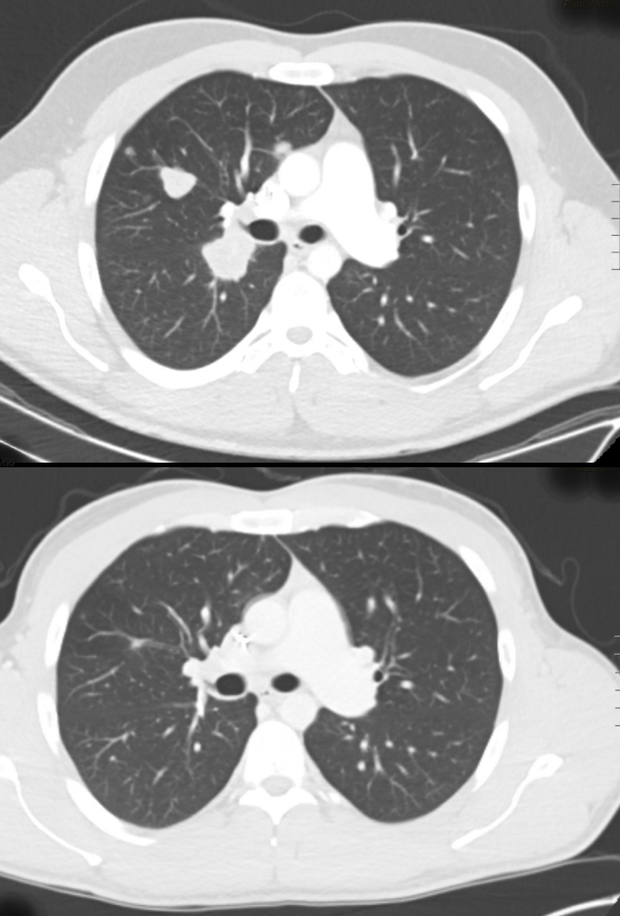
A young dad’s colon cancer spread to his lungs with no warning. He says a clinical trial led to a miracle.

Spencer Laird first noticed blood in his stool when he was 25. His doctor thought it was hemorrhoids caused by his work as a mechanic. Eighteen months later, a colonoscopy found colorectal cancer, which was treated with a surgery that removed 16 inches of his colon.
Two years passed, and Laird began to believe the worst was behind him. He returned to work and treasured time with his young daughter. Then his wife CarleyAnn Laird raised a concern at a routine follow-up appointment in December 2024.
“They had already checked out everything and said ‘Everything looks good to go.’ And she said, ‘No, he’s been sleeping a lot lately, he’s been tired a lot.’ She told him that she wanted him to do a full body scan on me,” said Laird, who lives in South Carolina.
He was surprised by the suggestion. He felt fine. But a scan showed that Laird’s cancer had returned — and spread. There were 13 tumors in his lungs. One was the size of a golf ball. His doctor said Laird would likely have only about two years to live, even with treatment.
“So much went through my head,” Laird said. “I just thought: I’m 30 years old. I’ve got a wife. I’ve got a 5-year-old little girl. There was the shock of it.”
Spencer Laird
Joining a clinical trial with “nothing to lose”
Laird was diagnosed with microsatellite stable colorectal cancer, which is typically treated with chemotherapy and radiation. Laird had never wanted to undergo chemo. Dr. Michael James Overman, an oncologist and researcher at the University of Texas MD Anderson Cancer Center who was not involved in Laird’s care, said chemotherapy can control disease for at least six months for about 80 to 90% of microsatellite stable colorectal cancer patients.
Still, hearing that it was recommended was disheartening for Laird. He worried about the side effects and his quality of life, especially since his disease was considered terminal. CarleyAnn, a pharmacy technician, began looking for other options.
“I stayed up days and just stared at his scans,” CarleyAnn said. “This was strictly me not wanting to lose my husband and having to tell my 5-year-old.”
She applied to several clinical trials on her husband’s behalf, including one at Duke University where gastrointestinal oncologist Dr. Nicholas DeVito was studying the effects of immunotherapy on microsatellite stable colorectal cancer. Typically, immunotherapy has been used to treat this kind of cancer after multiple forms of chemotherapy have failed, DeVito said. A previous clinical trial showed that when it was used as a “fourth or fifth line of defense,” there were “nice responses in about a quarter of patients,” DeVito said. The study showed that the immunotherapy controlled the disease — meaning tumors either shrank or stayed the same size — in 70% of patients.
Shawn Rocco/Duke Health
Devito’s trial tests what happens when immunotherapy is used first, without chemotherapy. Delaying chemo can be risky, DeVito said, so patients whose disease may interfere with organ function are not eligible.
Laird said the potential benefits outweighed his concerns.
“I don’t like to say you have nothing to lose, but that’s kind of the only way to put it,” Laird said. “When you get a diagnosis like that, why not try something that you don’t know anything about?”
“A miracle from God”
Laird became one of 15 patients enrolled in the trial in February last year. Patients receive an immunotherapy infusion every two weeks, DeVito said. Scans are taken every six to eight weeks to monitor their disease. If a patient starts to show signs of disease progression, they start chemotherapy.
Scans showed Laird’s tumors “melting away,” DeVito said. He went from 13 tumors to three. The largest is just 0.6 millimeters — significantly smaller than the golfball-sized tumor that his doctor had first detected.
Duke Health
“It’s a miracle. It’s really a miracle from God,” said Laird. “Looking at where it started and where it is now, it’s just unbelievable.”
Laird had some side effects, including rashes, headaches, nausea and dizziness during the early days of the treatment, but they abated in late spring 2025. Overman said that like chemotherapy, immunotherapy can have some toxicity. Since then, it has been “smooth sailing,” CarleyAnn said, with her husband only occasionally experiencing some stomach troubles.
Laird had one of the strongest responses early on, DeVito said. The full results of the trial will be published in April.
“In a nutshell, this was a diagnosis that would probably have shortened his life to five years or less, at best,” DeVito said. “And now we’re thinking ‘Well, is he cured? How long does this remission last? Is it permanent? How does this cancer stay away?’ We’re really drifting into uncharted territory.”
Shawn Rocco/Duke Health
A “first in history”
While Laird may be a “first in history,” DeVito said he hopes to identify more patients who can have the same success. That may help researchers identify which patient populations should get immunotherapy as a first-line treatment. Further research may also look like at combining the immunotherapy with other treatments.
Overman said the trial is novel, but that there is still a long way to go before early immunotherapy can be considered a standard of care treatment for microsatellite stable colorectal cancer. Future research should investigate if there are patients with certain biomarkers may respond better to immunotherapy than others, he said. Experts may also continue to refine patient selection in future trails. Primary tumors tend to be more immune responsive and may react to immunotherapy better, Overman said, as opposed to someone whose cancer has metastasized. Still, it may provide an option for patients who don’t want chemotherapy.
“This here is proof of concept. You can do it front line, and there’s definitely some activity,” Overman said. “We don’t have a lot of non-chemo approaches. That’s the real novel aspect here.”
Laird is not cancer-free, but his disease is no longer terminal. He continues to visit Duke every two weeks for an infusion infusion. CarleyAnn said family and their church parish have offered essential support. Laird said the experience has encouraged him to treasure every moment.
“It really just taught me to try to live life,” Laird said. “There’s no sense sitting around being lazy. If the good Lord wakes you up every day and you got breath in your lungs, just go do something.”